As physicians, the patient-encounter is a routine process that we hardly analyze in a scientific manner. But the physician-patient encounter is extremely important from the perspective of health management information systems. Though the workflow and thought-flow may vary based on the setting, individual and specialty, I have tried to summarize basic steps in a physician-patient encounter.
Initially there will be a rapport building phase for new patients which naturally will be unstructured. This is followed by history taking and clinical examination. A physician may take notes during this process, but the information on his notes generally will be semi-structured. This information is transcribed into the EMR in a fully structured form though free form text may be needed to capture certain elements.
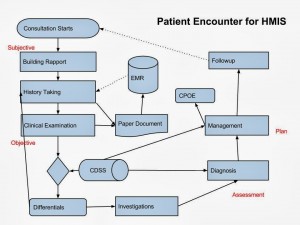 |
The physician arrives at a list of probable diagnosis (differentials) following which the physician may go back to history taking and examination to find more clues for a definitive diagnosis. Clinical decision support systems (CDSS) may be useful during this phase. Physician requests investigations and comes to a more specific diagnosis.
Management starts with a specific diagnosis in most cases. CDSS helps during this phase along with computerized physician order entry (CPOE) and ePrescription. When the patient comes for follow-up, these steps are repeated and the initial diagnosis is re-evaluated.
- Word to LaTeX: How paperajcli Bridges Two Academic Worlds - May 5, 2026
- When GenAI Ideas translate to practice with DHTI - March 4, 2026
- How DHTI Makes MCP Practical for Healthcare Through “Docktor” (Part IV) - February 4, 2026
